If you’ve ever rubbed the base of your skull after a long day at a desk and thought, “This must be my posture,” you’re not imagining things — but the full story is a bit more nuanced.
Posture can absolutely contribute to headaches, especially when paired with long hours of sitting, stress, poor sleep or a sudden increase in workload. But posture is rarely the only driver. For many people, headaches are a mix of neck mechanics, muscle endurance, nervous system sensitivity and lifestyle load.
The good news: when neck and upper back factors are part of the picture, physiotherapy can make a meaningful difference — particularly for cervicogenic headaches and some tension-type headaches.
TL;DR
- Posture may contribute to headaches, but it’s usually one piece of a bigger puzzle.
- Neck and shoulder endurance, stress and sustained positions often matter more than a “perfect posture.”
- Physio can help by calming pain, restoring movement and building long-term resilience with targeted exercise.
Why posture gets blamed (and why that’s not the whole story)
“Bad posture” is an easy culprit because it’s visible — and because many headaches flare after long periods of sitting or screen use.
But modern evidence and clinical experience suggest a better framing:
it’s not posture itself — it’s prolonged, sustained posture without enough movement variety or strength capacity.
In other words, your body might tolerate a position for 5–10 minutes… but not for 5–10 hours.
Headache types where neck and posture can matter
Not all headaches are the same. Understanding the likely pattern helps guide what treatment is most useful.
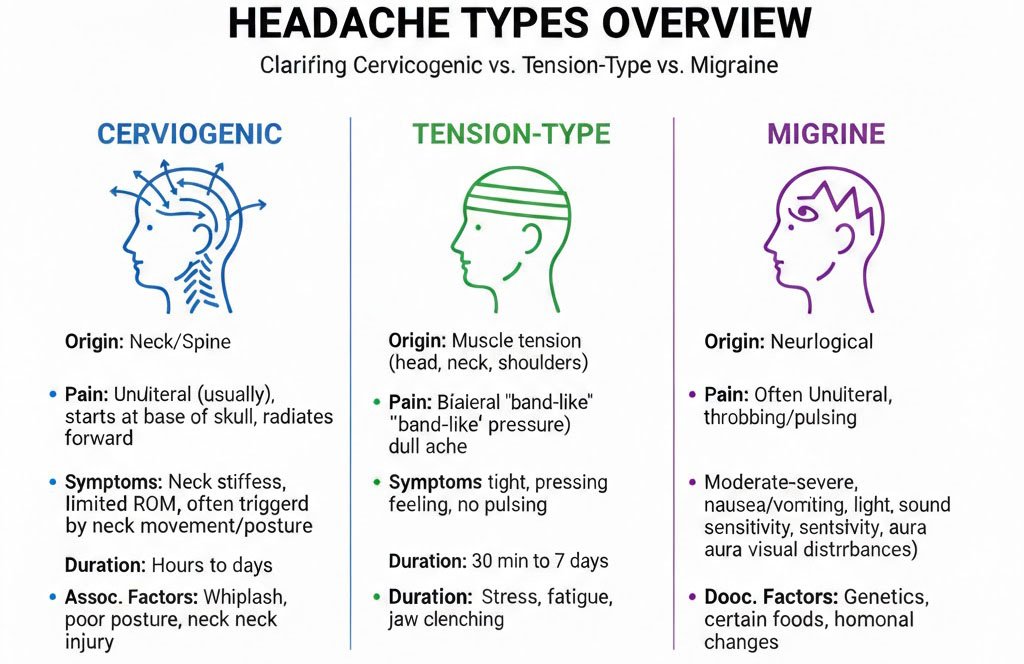
1. Cervicogenic headache (neck-related)
This type is driven by structures in the upper neck. Common cues include:
- Pain that often starts in the neck then spreads into the head.
- Headache that can be linked to neck movement or sustained positions.
- Neck pain alongside the headache.
Physio is frequently part of management, with a combination of education, manual therapy and exercise.
2. Tension-type headache
This is very common and can present with:
- A “tight band” or pressure feel around the head.
- Neck and shoulder tightness.
- Symptoms that worsen with stress, fatigue and long desk days.
Physio may help reduce intensity and improve function, especially when neck/shoulder factors are present.
3. Migraine (sometimes with neck involvement)
Migraines are more complex neurologically, but neck discomfort can still be part of the pattern. A physio approach is usually supportive and integrated with GP management.
Signs your headache might be posture/neck-influenced
You may benefit from a physiotherapy assessment if you:
- Notice headaches after long screen time or driving.
- Feel neck stiffness before the headache starts.
- Get relief when you move, stretch or change positions.
- Experience headaches alongside reduced neck range of motion.
- Have recurring tightness in upper traps, suboccipitals or jaw muscles.
How physiotherapy can help
A good physio plan focuses on clarity + capacity, not just quick relief.
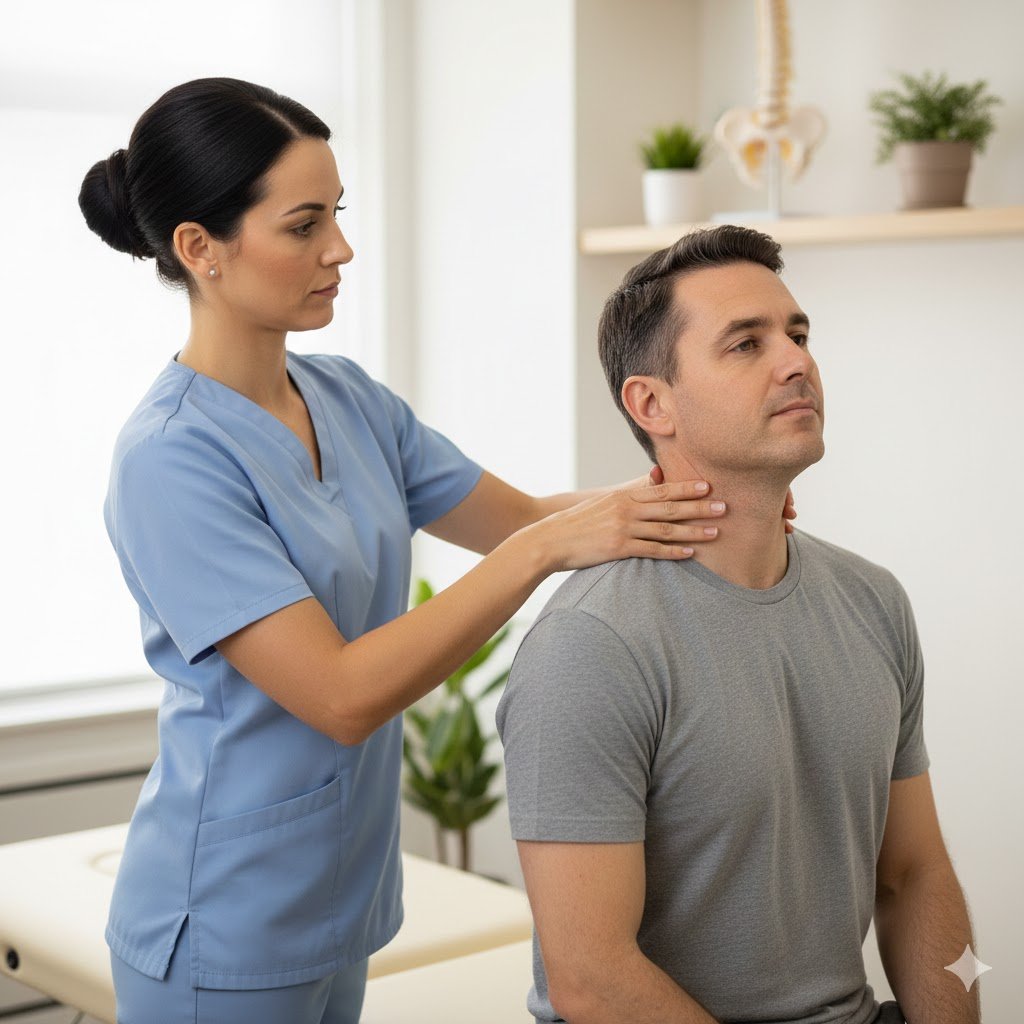
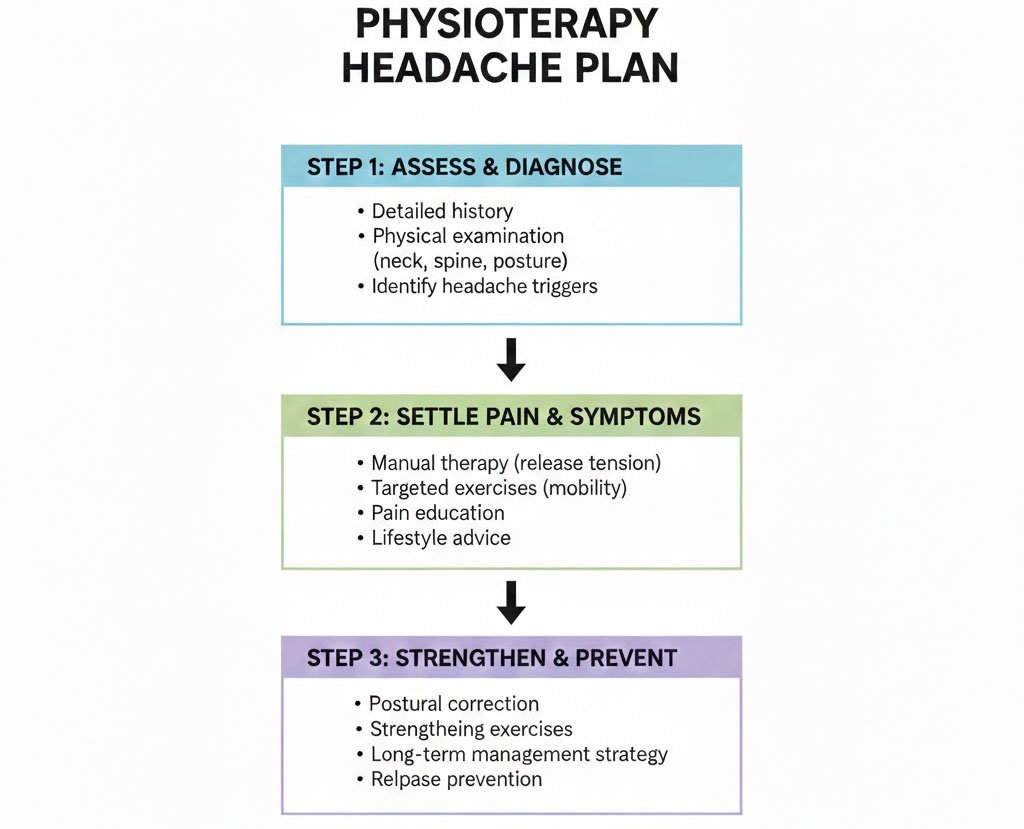
What you can expect in a posture-headache plan
1) Clear assessment
Your physio will look at:
- Headache pattern and triggers
- Neck and upper back mobility
- Deep neck flexor endurance
- Shoulder blade control
- Daily load: sleep, stress, training, working positions
- Jaw/TMJ contribution if relevant
2) Symptom settling
Depending on your presentation, this may include:
- Gentle manual therapy for the upper neck and surrounding muscles
- Soft tissue work for jaw/neck/shoulder tension where appropriate
- Education to reduce fear and over-guarding
Manual therapy can help short-term comfort and may support a more active rehab approach.
3) Strength + endurance that actually sticks
This is often the long-term game changer. Programs commonly involve:
- Deep neck flexor activation and endurance
- Scapular and upper back strength
- Thoracic mobility drills
- Graded exposure to desk, gym and sport demands
Exercise-based interventions show promise for reducing headache burden, especially in neck-influenced patterns.
Step-by-step: simple posture habits that help
These are not magic fixes — but they can reduce load on sensitive tissues.
Try this daily rhythm
- Every 30–45 minutes: stand, walk or reset your neck/shoulders.
- Screen height: aim for eye level where practical.
- Keyboard/mouse: keep shoulders relaxed, elbows supported.
- Breathing check: soften jaw, drop shoulders, slow exhale.
Small, repeatable changes beat a short-lived “perfect posture” attempt.
Common mistakes
You don’t need to wait weeks to ask for help.
Myths vs facts
Myth: Bad posture is the main cause of headaches.
Fact: Posture is often a contributor, not the whole diagnosis.
Myth: If I just strengthen my neck once a week, it will fix it.
Fact: Consistency and progressive loading matter most.
Myth: Headaches are always “just muscular.”
Fact: Headaches can involve nervous system, stress and lifestyle factors too.
A short example
You spend long hours on a laptop. You’ve developed:
- Neck stiffness
- Shoulder tightness
- Headaches 2–3 afternoons per week
A physio plan might focus on:
- Improving upper neck mobility
- Building deep neck flexor endurance
- Strengthening scapular support
- Adjusting your work “movement rhythm”
- A graded return to gym loads
Over time, the goal is a neck that can handle your real life without constantly flaring.

FAQs
Yes — especially when neck joints and muscles are overloaded by sustained positions. But it’s usually one factor among others like stress, sleep or training load.
Cervicogenic headaches are driven by the upper neck and often begin there, while tension-type headaches are more widespread and can be influenced by muscle tension and stress. A physio assessment helps clarify which pattern fits best.
Not usually. Many headache patterns can be assessed clinically first. Imaging may be suggested if your symptoms or history indicate it could change management.
Seek prompt medical review if you have:
Headaches after a significant head/neck injury
- A sudden severe “worst ever” headache
- New neurological symptoms (weakness, speech changes, vision loss)
- Fever, neck stiffness or confusion
- A new headache pattern after age 50
- Headaches after a significant head/neck injury
Some people feel early relief within a few sessions, but meaningful, lasting change usually comes from building strength and endurance over weeks.
Key takeaways
- Posture often contributes to headaches — but rarely explains everything.
- The real goal isn’t perfect posture; it’s better capacity + more movement variety.
- Physio can help reduce symptoms and build long-term resilience, especially for neck-related and some tension-type headaches.
Conclusion
If your headaches tend to show up after long desk days, driving, or when your neck feels stiff and overloaded, there’s a strong chance a neck-and-posture-informed physio plan could help.
You don’t need to brace yourself into a “perfect posture.” You need a body that can handle your work, stress and routine — with less irritation and more confidence.

