A little leakage when you laugh. A sudden urgent dash to the toilet. A heavy or “dragging” feeling late in the day.
Many women quietly put up with pelvic floor symptoms for years because they assume it’s normal after having kids, normal with age, or just something you have to live with. But common doesn’t mean harmless — and it definitely doesn’t mean untreatable.
Pelvic floor symptoms are often your body’s way of saying it needs support. With the right assessment and a tailored plan, physiotherapy can help many women improve bladder control, reduce discomfort, and rebuild confidence in everyday movement. Pelvic floor muscle training is widely recommended for urinary incontinence and has strong evidence behind it.
TL;DR
- Pelvic floor symptoms are common, but they’re not something you should just “push through.”
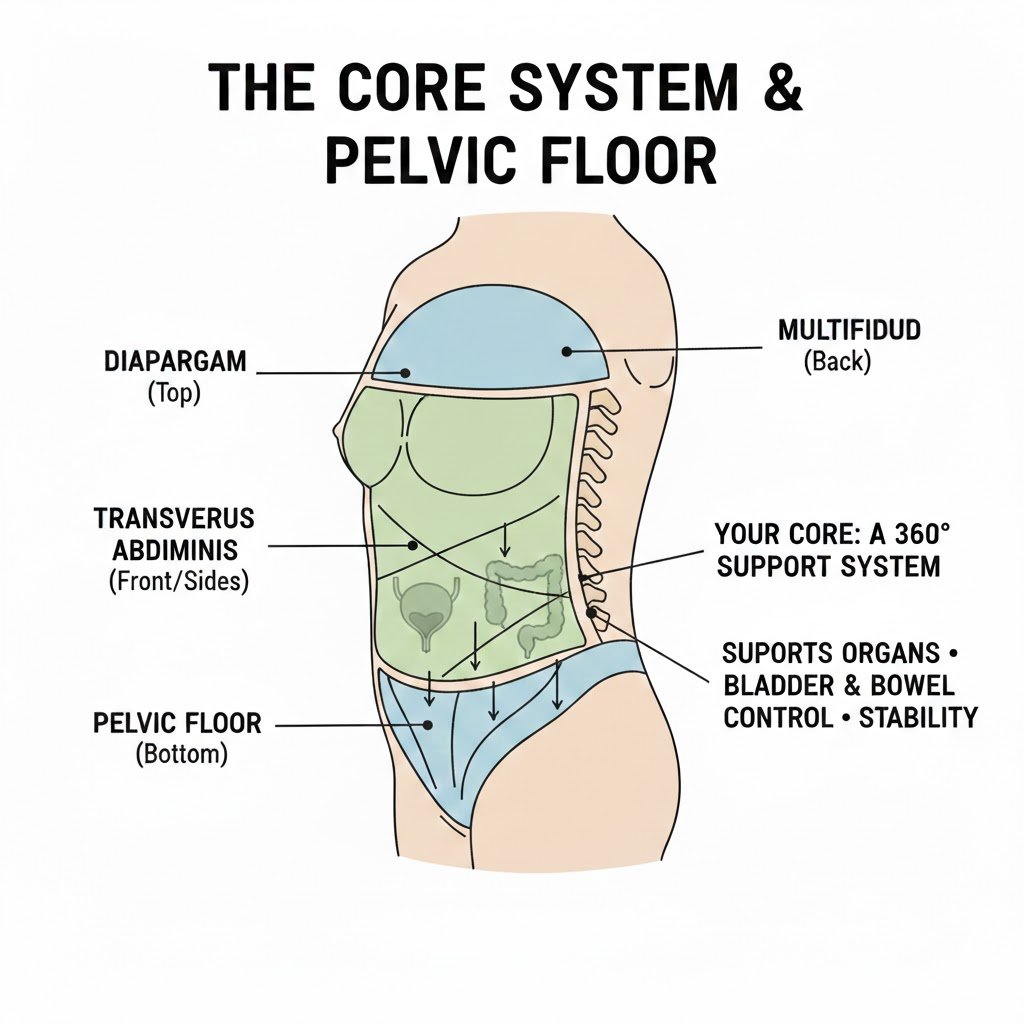
- The pelvic floor is part of your core system and supports bladder, bowel and pelvic organ function.
- Physiotherapy can help improve control, strength, relaxation and coordination — and often reduces leakage with consistent training.

What the pelvic floor actually does (and why it matters)
Your pelvic floor is a layered group of muscles and connective tissue that forms the base of your pelvis. It helps:
- support pelvic organs
- control urine, bowel and wind
- contribute to sexual function
- work with your diaphragm and deep abdominal muscles as part of the core system.
When this system is struggling — too weak, too tight, poorly coordinated, or overloaded — symptoms can show up in ways that affect daily life.
Common pelvic floor symptoms women shouldn’t ignore
Pelvic floor issues aren’t one-size-fits-all. You may notice:
Bladder symptoms
- Leaking when you cough, sneeze, laugh or exercise (stress urinary incontinence).
- Strong urgency or frequent urination.
- Feeling like you can’t fully empty your bladder.
Pelvic organ support symptoms
- A sense of heaviness, pressure or bulging in the vagina.
- Symptoms that worsen after standing, lifting or long days.
Bowel symptoms
- Constipation or straining
- Difficulty controlling wind or bowel urgency
Pain and sexual function
- Pelvic, vaginal or lower back pain
- Pain with intercourse
- Jaw/hip/low back tension patterns that often travel with pelvic floor overactivity
(These symptoms can have multiple causes — which is exactly why assessment matters.)
Why ignoring symptoms can make recovery harder
A lot of women wait until symptoms become disruptive. The problem is that small changes can often be easier to address early — before compensation patterns and confidence loss build up.
Delaying support may lead to:
- reduced activity and exercise avoidance
- worsening strength and endurance
- increased fear around movement
- progression of symptoms across life stages (pregnancy, postnatal, perimenopause/menopause)
Postnatal pelvic health is a clear example. The Australian Physiotherapy Association highlights the importance of early identification of birth-related pelvic health issues and recommends a postnatal physiotherapy consultation around six weeks after birth, with access often needed up to 12 months or more.
The “posture” myth equivalent in pelvic health
Just like headaches get blamed on “bad posture,” pelvic floor symptoms often get blamed on one cause — usually childbirth.
Childbirth is a major factor, but it’s rarely the only one. Pelvic floor symptoms can also be influenced by:
- chronic constipation or straining
- heavy or sudden increases in lifting
- persistent coughing
- hormone changes
- high-impact sport without adequate pelvic floor capacity
- poor breathing/pressure strategies
These load factors are acknowledged in Australian consumer resources on pelvic floor health.

How physiotherapy helps
Pelvic health physiotherapy is not just “do some Kegels.” The best care is precise, respectful and personalised.
1) Clear assessment
Your physio may assess:
- your symptom pattern and triggers
- pelvic floor strength, endurance and coordination
- breathing and pressure control
- hip, trunk and general strength
- toileting habits and lifestyle factors
2) The right type of training (not always more squeezing)
Some women need:
- strength and endurance building
Others need: - down-training (learning to relax overactive muscles)
- better coordination with breathing and movement
This is why correct diagnosis matters. An overactive pelvic floor can sometimes mimic weakness — and doing the wrong approach can be frustrating.
3) Evidence-based pelvic floor muscle training
For urinary incontinence, pelvic floor muscle training is a first-line treatment. Women with stress urinary incontinence doing PFMT are reported to be several times more likely to feel cured or improved compared with no treatment.
Clinical guidance commonly recommends structured daily training with progressive positions and effort over time.
4) Practical strategies for daily life
A good plan also includes:
- lifting and exercise modifications
- return-to-running or gym progression
- bladder/bowel habit support
- education that reduces fear and shame
Step-by-step: a simple starting framework
This is not a substitute for individual care, but it’s a safe way to think about your next step:
1) Notice your pattern
- When does leakage or heaviness show up?
- What makes it better or worse?
2) Reduce aggravators briefly
- High-impact spikes
- Straining with constipation
- Rushing heavy loads without breath control
3) Book a pelvic health assessment
You’ll get clarity on whether you need strength, relaxation, or both — plus a plan that fits your life.
Common mistakes
You don’t need to wait weeks to ask for help.
- Assuming symptoms are “normal” because they’re common.
- Doing random pelvic floor exercises without knowing if the muscles are weak or overactive.
- “Testing” your pelvic floor by frequently stopping urine mid-stream (this should be used sparingly, if at all, and only as instructed). (Department of Health)
- Ignoring constipation and breath/pressure habits.
Myths vs facts
Myth: Leaking after childbirth is just something you accept.
Fact: Many women improve significantly with the right physiotherapy plan.
Myth: Kegels fix everything.
Fact: Some women need relaxation and coordination first.
Myth: Pelvic floor issues only affect older women.
Fact: Symptoms can occur across life stages — including pregnancy, postnatal and high-impact sport.
A short example
You’re six months postnatal and notice:
- mild leaking with jogging
- a heavy feeling by afternoon
- difficulty reconnecting with your core during lifting
A physio plan might include:
- pelvic floor + deep abdominal coordination
- graded strength and endurance
- pressure management for lifts
- a staged return-to-running plan
This is exactly the kind of scenario where early support can prevent long-term frustration.

FAQs
Bladder leakage, urgency, pelvic heaviness or pressure, constipation/straining, and pelvic pain are common reasons women seek pelvic health support.
It’s common, but that doesn’t mean you should ignore it. Many women improve with a tailored pelvic floor and core program, especially when started early.
Yes. Pelvic floor muscle training is a leading non-surgical approach, with strong evidence showing meaningful improvement for many women.
That’s common. Overactivity can cause pain, urgency and difficulty relaxing. A pelvic health physio can guide down-training and coordination before progressing strength work.
For private appointments, usually no. If you’re using Medicare CDM, you’ll need a GP management plan and referral.
See a GP promptly if you have:
- blood in urine
- fever or signs of infection
- new sudden inability to control bladder/bowel
- significant unexplained pelvic pain
concerning vaginal bleeding or rapid symptom change
Key takeaways
- Pelvic floor symptoms deserve attention early, not later.
- The pelvic floor is part of your core and impacts bladder, bowel and pelvic organ support.
- Evidence-based physio can help many women improve control, comfort and confidence.
- The right plan depends on whether your pelvic floor needs strength, relaxation, or both.
Conclusion
Pelvic floor symptoms can be quiet at first — a small leak here, a little heaviness there — but they often carry a disproportionate emotional load. They affect how you move, how you exercise, how you socialise, and how you feel in your body.
You don’t need to wait until things get worse to seek help. With an assessment and a structured plan, many women see real improvements in bladder control, core confidence and everyday comfort.

